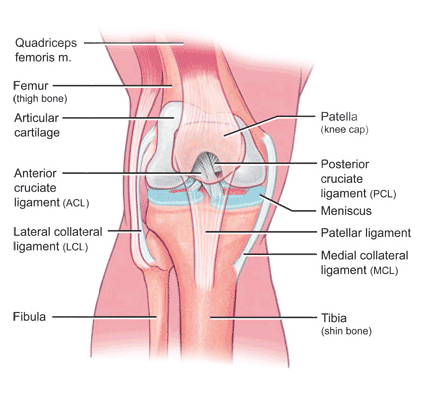
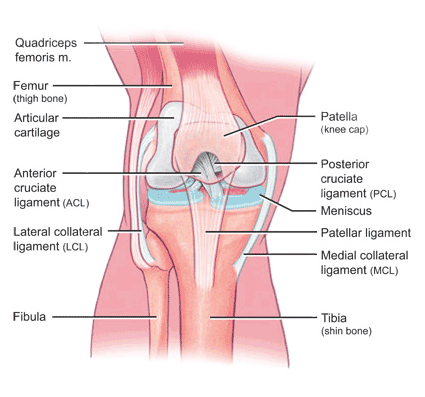
I was operating upon a fellow with a serious knee injury last week. It required the reconstruction of not just one but several ligaments. The matter had come to my attention by referral of one of our associated physiotherapists, from Powerhouse Physiotherapy in Canberra.
You might be interested to know how I manage acute severe knee injuries.
Things have definitely changed over the last 5 years and we, as ever, are right at the forefront of this technology.
If someone presents with an injury to the anterior cruciate ligament, in isolation, then the usual recommendation is to manage the instability by using an autograft. This refers to using a tendon harvested from the person, on the day. Occasionally, we use tendons from others, called allografts but this is not the usual, first line option.
When there is more complexity, say with a combination of a tear of the ACL and the MCL (medial collateral ligament), we usually manage the ACL, and subsequently, at the same operation, assess the MCL. As the knee is meant to be stable on the inner (medial ) side, we place increasing emphasis on making sure that this is stable.
If there is significant residual instability, then we would stabilise this area, often using an artificial graft over the top of the MCL that we have also reconstructed.
Why do I do this? The reason lies in the fact that the MCL has a very good blood supply and, given a little support, at the right length, will heal at the correct tension. This can usually be done in such a way that patients do not need to wear a knee brace after the surgery. Crutches and some degree of partial weight bearing are usually needed for a short period of time, say 3 weeks, but we get people into the pool for rehabilitation as soon as we can, often 2 weeks after surgery.
The benefit of this is to allow immediate mobilisation of the joint, to the distinct benefit of the patient whose muscle strength definitely increases much more quickly than if they are in a knee brace. People don’t like knee braces!
We use this principle for other ligaments as well, like injuries to the postero-lateral corner of lateral collateral ligament. The benefits of more rapid recovery and better stability are clear.
The old days of just leaving the MCL to heal itself are changing, partly predicated upon the knowledge of the true way in which the knee works. This was clarified by Professor Michael Freeman and co-workers. They found that the knee is normally perfectly stable on the medial side and that the knee pivots around a central point in the knee joint whilst the lateral side moves back and forwards with much more freedom. This has been the basis for the medial pivot knee replacement that is gaining popularity both in my practice as well as world wide. It makes perfect sense; looking after the MCL also seems to make perfect sense.
